 You may notice a trend during the month of November where lots of normally clean-shaven blokes are suddenly sporting (often embarrassingly hideous) attempts at growing a moustache. There’s a good chance that they are making a spectacle of themselves for a worthy cause. Over the past sixteen years, the Movember Foundation has raised over a billion dollars globally to promote awareness of men’s health issues, including prostate cancer, testicular cancer, depression and suicide prevention. Last year, participants in Australia alone raised $29 million. More than 75% of the money raised is used to fund at least 1250 men’s health projects, including Beyond Blue and the Prostate Cancer Foundation of Australia.
You may notice a trend during the month of November where lots of normally clean-shaven blokes are suddenly sporting (often embarrassingly hideous) attempts at growing a moustache. There’s a good chance that they are making a spectacle of themselves for a worthy cause. Over the past sixteen years, the Movember Foundation has raised over a billion dollars globally to promote awareness of men’s health issues, including prostate cancer, testicular cancer, depression and suicide prevention. Last year, participants in Australia alone raised $29 million. More than 75% of the money raised is used to fund at least 1250 men’s health projects, including Beyond Blue and the Prostate Cancer Foundation of Australia.
For the past 12 years, I too have participated in one way or another in Movember, either by growing a mo’ myself or sponsoring others. This year I have joined the official Deloitte Platform Engineering (DPE) Movember team. My motivation has always come in part from my family’s history of prostate cancer: my dad and two of my three brothers have endured this disease. This year, I have even more inspiration, as I recently extended my family’s history via my own battle with prostate cancer. I will share a bit of my story below.
The Importance of Vigilance and Awareness
Prostate cancer is the 6th leading cause of death for males in Australia, ahead of all other cancers besides lung cancer. That’s a very sobering statistic and should be a warning beacon to all men. The only good news is that prostate cancer is about the slowest growing cancer there is – so if caught early, the prognosis for a complete recovery is very good. The challenge is in actually detecting it. There are typically few noticeable symptoms prior to advanced stages of prostate cancer, so it is imperative to be proactively vigilant.
The most common form of screening is via a prostate-specific antigen (PSA) blood test. A higher score on this test can be an indicator of prostate cancer. However, this is not foolproof, as cancer doesn’t always result in a high PSA count, nor does a higher count always mean there is cancer present. In addition, scores are relative to your age (as you get older your PSA count will likely rise). A spike in your PSA count is a more likely indicator of a problem, and this will typically prompt a further investigation.
PSA tests are less invasive and uncomfortable than a digital rectal exam (DRE), but a combination of both may be recommended if you are considered at risk (i.e. having a family history of prostate cancer). A DRE will detect a swollen prostate, whilst a PSA test obviously cannot. Swelling or hardness of the prostate can be a sign of cancer, which may cause a doctor to recommend an MRI scan and possibly a biopsy. Another sign of a prostate swelling is a weakening urinary stream.
If recommended, a biopsy will be performed in a hospital as a day procedure. Small samples of tissue are extracted from the prostate and examined for cancerous growth. There are two types of biopsies performed today: TRUS and transperineal. The latter requires general anaesthetic but is usually the preferred approach as it can produce better samples and has a lower risk of infection. The areas targeted for sampling are usually identified by previous scans such as an MRI. If cancerous tissue is found in the sample, then a definitive prognosis can be made and a course of treatment recommended. But if no abnormal tissue is found, this does not necessarily mean you are cancer free, as the samples could have missed the affected area.
My Experience
Because of my strong family history, I faithfully had a PSA test every year, sometimes accompanied by a DRE as well. Over the course of time it would climb a little bit, but usually within expected margins. However, my test this past March was about two points higher than last year, a slightly more dramatic increase. My GP then performed a DRE and ordered an ultrasound to see if there was any abnormal swelling. Nothing unusual was found, so we decided to leave it and wait until next year’s PSA test.
A few weeks later, I asked of my own accord to have a full blood test performed – for a very different reason. It had been a stressful couple of years, and I was frequently feeling fatigued. A friend of mine suggested having my vitamin levels checked. This turned out to be a life saving move for me. I wasn’t even aware that a PSA test would be included in the analysis, so I was surprised when the GP announced that my PSA had jumped up a further three points in as many weeks! This triggered a referral to a urologist, who requested an MRI in advance of my initial appointment.
The MRI and a more thorough DRE performed by the urologist confirmed an abnormal hardening and protrusion, therefore we scheduled a transperineal biopsy. On the day of the procedure, a very competent anaesthetist gave me the best sleep I’d had in months – at least for a couple of hours. 😉 I was surprised that there was really no pain or discomfort afterwards, just some expected traces of blood in the urine for a few days.
The pathology confirmed that I had a very aggressive cancer (Gleason score of 9!), and there was evidence it may have reached the outer wall of the prostate. Therefore, the urologist ordered a PSMA PET scan to determine if the cancer had metastasised (i.e. travelled elsewhere in the body). Thankfully, the scan showed no sign of this. Given my age and other factors, he recommended a radical prostatectomy and scheduled my surgery in mid-July. (There is usually at least a 4-week interval before a proctectomy to allow post-biopsy prostate swelling to diminish, making it easier to remove. It also allows time to facilitate the recovery process by performing pelvic floor exercises.)
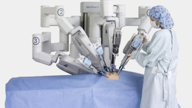 Surgery involved another couple of hours of awesome sleep (thank you, Mr. Anaesthetist!). As they wheeled me into the theatre and just before I went under, I caught a glimpse of the Da Vinci machine, an amazing piece of robotic technology that was used to perform the laparoscopic (“keyhole”) surgery. Six small holes in my abdomen area was all that was needed thanks to this remote-controlled device.
Surgery involved another couple of hours of awesome sleep (thank you, Mr. Anaesthetist!). As they wheeled me into the theatre and just before I went under, I caught a glimpse of the Da Vinci machine, an amazing piece of robotic technology that was used to perform the laparoscopic (“keyhole”) surgery. Six small holes in my abdomen area was all that was needed thanks to this remote-controlled device.
By all counts the surgery was a success! The prostate came out easily, and the pathology proved that a healthy margin was obtained. This was a huge relief given the cancer’s aggressiveness, its breach of the outer wall, and its invasion into the seminal vesicle. Recovery was also swift. Although the overnight in the hospital was uncomfortable and largely sleepless (mostly due to the nurses’ obligatory hourly temperature and blood pressure monitoring), I was back on my feet and able to go home the next day. Two days after the surgery, I was able to start a regime of 2 to 4 kilometre daily walks. There was minimal pain from the six 1cm wounds, sufficiently minor that I was able to ditch the painkillers within a few days. The worst part was the bloating from the CO2 gas they had inflated my belly with; that took a few days to subside. And of course, there was the catheter to deal with for a week. Nevertheless, I was back on the job a week after surgery (albeit working from home for a few weeks). The best news came three months later, when a follow-up blood test confirmed a PSA count of zero! I am now cancer free, praise God!!
Imagine if my friend had not prompted me to take the 2nd blood test! Given the aggressiveness of my cancer, waiting another 12 months for a PSA test would have been disastrous. I am thankful not only for this friend, but also for the skill of my urologist and his surgical team, for the technology that makes robotic assisted surgery possible, for family and friends who supported me and also for my Deloitte family – especially a few DPE superstars who surprised me with a huge delivery of YouFoodz meals, saving me the burden of cooking for a couple of weeks! This certainly was a fine example of one of Deloitte’s core values: take care of each other.
As you might expect, my involvement in Movember this year will be the most personally significant to date!
What Can You Do?
If you’re a male over 50 years of age, consider having a PSA test every two years. If there is any history of prostate cancer in your family, maybe start at 40 years old. Either way, talk to your GP about an appropriate approach to vigilance. Early detection is critical with any cancer, and with prostate cancer it ensures a very high success rate for total cure.
Whether you are male or not, you can certainly assist others by supporting the Movember Foundation. Simply have some sympathy for your colleagues’ embarrassing attempts at  growing facial hair. You can start by supporting the official DPE Move & Tash team with a pledge to the entire team, or to an individual team member like myself. You can also support the 2019 Deloitte Stair Climb Challenge, one of many initiatives of the Deloitte Foundation. Your donation helps the Movember Foundation raise awareness of prostate cancer and contributes to the research and technology that made my diagnosis, treatment and recovery possible!
growing facial hair. You can start by supporting the official DPE Move & Tash team with a pledge to the entire team, or to an individual team member like myself. You can also support the 2019 Deloitte Stair Climb Challenge, one of many initiatives of the Deloitte Foundation. Your donation helps the Movember Foundation raise awareness of prostate cancer and contributes to the research and technology that made my diagnosis, treatment and recovery possible!
Finally, if you find yourself facing a possible diagnosis of prostate cancer, please feel free to contact me as I will be happy to share more details of my experience and provide firsthand information on what to expect.

